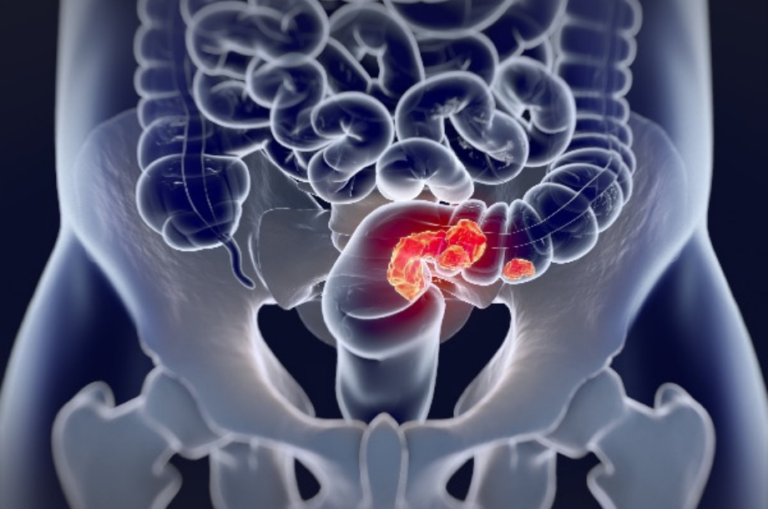
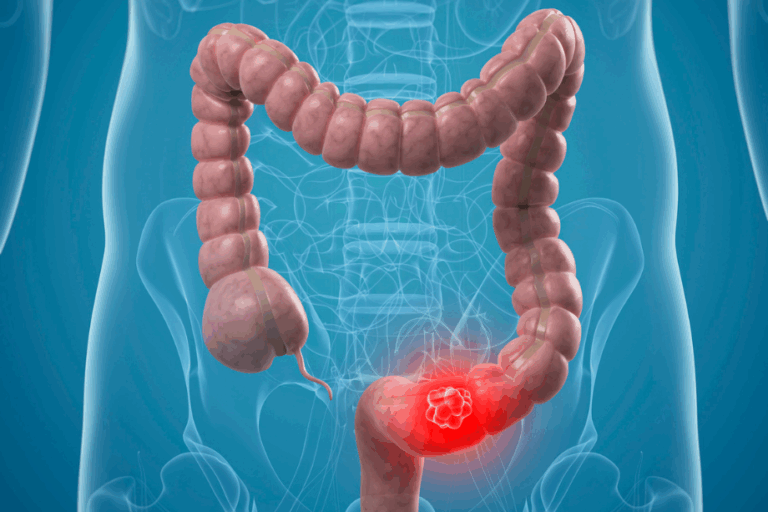
Not long ago, colon cancer was mostly seen in people over 70. But today, about 1 in 10 new cases are in people under 50. In fact, colon cancer is now the number one cause of cancer deaths in men under 50, and the 2nd most common in women under 50. This isn’t just an American problem—it’s happening worldwide.
Why Early-Onset Cancer is Different
Colon cancer diagnosed before age 50 is called early-onset. The tricky part is that doctors and patients don’t expect it in younger people, so it’s often caught late. That makes it more aggressive and harder to treat. Compared to later-onset, early-onset cancers often:
- Start in the left colon or rectum
- Spread (metastasize) sooner
- Have unique genetic patterns
Genetics play a bigger role here—30% of younger cases are tied to inherited risks (vs. only 10–15% in older adults). Yet, many young people with genetic risks don’t qualify for testing under current guidelines.
When Should You Get Screened?
Most people start routine colon cancer screening at age 45, but some need it earlier. You may need to get checked if you have:
- A parent, sibling, or child diagnosed before 60
- Two or more relatives with colon cancer at any age
- Symptoms like blood in stool, a change in your bowel habits, abdominal pain, unexplained weight loss, or fatigue
- Conditions like Lynch syndrome, Familial Adenomatous Polyposis (FAP), Crohn’s, or ulcerative colitis
- Multiple colon polyps
Screening options include:
- Colonoscopy – gold standard (can remove polyps on the spot)
- Stool tests like FIT (yearly) or Cologuard® (every 3 years)
- CT Colonography – “virtual” colonoscopy
- Flexible Sigmoidoscopy – less common and only looks at part of the colon but still an option
If any test other than colonoscopy is abnormal, you’ll still need a colonoscopy to confirm. As a gastroenterologist I strongly favor colonoscopy for screening because it can diagnose and remove polyps at the same time.